Wind Chill Explained |
What is Wind Chill Temperature?
It is the temperature it "feels like" outside and is based on the rate of heat loss from exposed skin caused by the effects of wind and cold. As the wind increases, the body is cooled at a faster rate causing the skin temperature to drop. Wind Chill does not impact inanimate objects like car radiators and exposed water pipes, because these objects cannot cool below the actual air temperature.
The term "wind chill" goes back to the Antarctic explorer Paul A. Siple, who coined it a 1939 dissertation, "Adaptation of the Explorer to the Climate of Antarctica." During the 1940's Siple and Charles F. Passel conducted experiments on the time needed to freeze water in a plastic cylinder that was exposed to the elements. They found that the time depends on how warm the water is at the beginning, the outside temperature and the wind speed.
Explanation
There is a thermal boundary layer surrounding the skin which may be several millimeters thick. This boundary layer acts as an insulator. When it is cold and the wind is blowing, the air feels colder than it does when it is calm because the wind blows away the boundary layer. In a perfect calm, if free convection could be suppressed (as it is in microgravity), the boundary layer would be infinitely thick. Add a wind, and the only still air that remains would be the air in the immediate vicinity of some surface, like the skin. The stronger the wind, the thinner the layer. Because the outer layers of still air are blown off more easily than the ones closer to the skin, when it is nearly calm, a small increase in wind speed causes a much greater thinning of the boundary layer thickness than the same increase in wind speed when the wind is already strong.
Convective heat loss is really conduction through an insulating boundary layer. The insulation of the boundary layer depends on its thickness. When there is wind, the thermal resistance of the boundary layer is smaller, the heat loss is higher, and the temperature of the skin is closer to the air temperature. Humans do not sense the temperature of the air but the temperature of the skin. Because skin temperature is closer to the air temperature when it is windy, the wind causes it to feel colder.
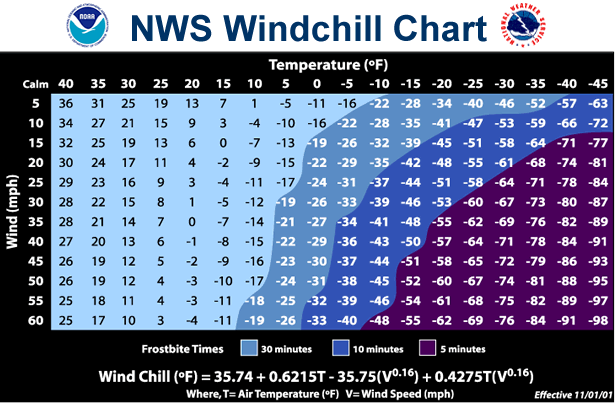
A wind-chill factor of 25°F (-4°C) will not freeze water if the air temperature is 35°F (2°C). Water state changes according to the temperature of the body of the water. In this case, the water and air temperature are about the same â too high to freeze water.
Significance
The concept of wind chill is of particular significance in very cold climates such as the Arctic and Antarctic, at high altitude, at high speeds, or in very high winds. In much of North America in winter, wind chill is forecast and reported by news media. To some degree, people make decisions as to how they will dress for outdoor activity, or whether they will take part in outdoor activity based on the wind chill. This has a potential economic impact on ski operators and other outdoor recreation areas, and to merchants. Schools use the wind chill forecast to decide whether to let students outside for recess or lunch in cold weather. Heart patients pay attention to the wind chill, to estimate the stress the weather might place on their circulatory systems to avoid problems. The military modifies its training exercises when wind chill reaches dangerous levels. It is of great importance to the survival of humans and animals and can even affect some machinery and heating systems.
What Does this Mean to Me?
The NWS will inform you when Wind Chill conditions reach critical thresholds. A Wind Chill Warning is issued when wind chill temperatures are life threatening. A Wind Chill Advisory is issued when wind chill temperatures are potentially hazardous.
What is Frostbite?
Frostbite (congelatio in medical terminology) is an injury to the body caused by freezing body tissue. At or below 32°F (0°C), blood vessels close to the skin start to narrow (constrict). This helps to preserve core body temperature. In extreme cold or when the body is exposed to cold for long periods, this protective strategy can reduce blood flow in some areas of the body to dangerously low levels. The combination of cold temperature and poor blood flow can cause severe tissue injury by freezing the tissue. The initial stages of frostbite is sometimes called "frostnip." The most susceptible parts of the body are the extremities such as fingers, toes, ear lobes, or the tip of the nose. If frostbite is not treated immediately then the damage and the frostbite become permanent. Nerve damage will occur due to oxygen deprivation.
Symptoms of Frostbite?
Symptoms of frostbite include a loss of feeling in the extremity and a white or pale appearance. Areas will turn discolored, purplish at first, and soon turn black. After a while nerve damage becomes so great that feeling is lost in the frostbitten areas. Blisters will also occur. If feeling is lost in the damaged area, checking it for cuts and breaks in the skin is vital. Medical attention is needed immediately for frostbite.
|
NWS Memphis 12-Hour Minimum Wind Chill Forecast The chart depicts the current 12-hour Minimum Wind Chill Forecast Click on the image to enlarge. |
|||

|
|||
Treatment of Frostbite?
To treat frostbite, move the victim to a warm location and seek medical help. Soak frostbitten areas in warm (not hot) water, or, if in the wilderness, warm by contact with the skin of a non-frostbitten person. Continue until the victim has regained sensation and movement in the afflicted region; this often follows great pain as the nerves thaw. Never rub, slap or shake the stricken region as ice crystals in the frostbitten skin will damage surrounding tissue. Follow the treatment with a period of constant warmth: refreezing following thawing worsens the damage. Infected open skin can lead to gangrene and amputation may be needed.
What is Hypothermia?
Hypothermia is abnormally low body temperature (below 95°F). Warning signs include uncontrollable shivering, memory loss, disorientation, incoherence, slurred speech, drowsiness, and apparent exhaustion. Detailed explanation of symptoms is below. Medical attention is needed immediately. If it is not available, begin warming the body SLOWLY.
The Three Stages of Hypothermia?
Normal body temperature in humans is 98.6°F (36.8°C). Hypothermia can be divided in three stages of severity.
Stage 1
Body temperature drops by 1.8-3.6°F (1-2°C) below normal temperature (95-96.8°F or 35-36°C). Mild to strong shivering occurs. The victim is unable to perform complex tasks with the hands; the hands become numb. Blood vessels in the outer extremities constrict, lessening heat loss to the outside air. Breathing becomes quick and shallow. Goose bumps form, raising body hair on end in an attempt to create an insulating layer of air around the body (which is of limited use in humans due to lack of sufficient hair, but useful in other species). Often, a person will experience a warm sensation, as if they have recovered, but they are in fact heading into Stage 2. Another test to see if the person is entering stage 2 is if they are unable to touch their thumb with their little finger; this is the first stage of muscles not working.
Stage 2
Body temperature drops by 3.8-7.6°F (2-4°C). Shivering becomes more violent. Muscle mis-coordination becomes apparent. Movements are slow and labored, accompanied by a stumbling pace and mild confusion, although the victim may appear alert. Surface blood vessels contract further as the body focuses its remaining resources on keeping the vital organs warm. The victim becomes pale. Lips, ears, fingers and toes may become blue.
Stage 3
Body temperature drops below approximately 89.6°F (32°C). Shivering usually stops. Difficulty speaking, sluggish thinking, and amnesia start to appear; inability to use hands and stumbling is also usually present. Cellular metabolic processes shut down. Below 86.0°F (30°C), the exposed skin becomes blue and puffy, muscle coordination becomes very poor, walking becomes almost impossible, and the victim exhibits incoherent/irrational behavior including terminal burrowing or even a stupor. Pulse and respiration rates decrease significantly, but fast heart rates (ventricular tachycardia, atrial fibrillation) can occur. Major organs fail. Clinical death occurs. Because of decreased cellular activity in stage 3 hypothermia, the body will actually take longer to undergo brain death.
Treatment for Hypothermia
Treatment for hypothermia consists of drying, sheltering, and gradually warming (making sure to not rub the patient's body, to warm with blankets and, if possible, to transfer your own body heat). While blankets help a person retain body heat, they are not sufficient to treat hypothermia. It is vital that you warm the core of the body first or the cold blood will be forced towards the heart and may cause death. In the field, a mildly hypothermic person can be effectively rewarmed through close body contact from a companion and by drinking warm, sweet liquids.
Moderate and severe cases of hypothermia require immediate evacuation and treatment in a hospital. In hospital, warming is accomplished by external techniques such as heated blankets for mild hypothermia and by more invasive techniques such as warm fluids injected in the veins or even lavage (washing) of the bladder, stomach, chest and abdominal cavities with warmed fluids for severely hypothermic patients. These patients are at high risk for arrhythmias (irregular heartbeats), and care must be taken to minimize jostling and other disturbances until they have been sufficiently warmed, as these arrhythmias are very difficult to treat while the victim is still cold.
An important tenet of treatment is that a person is not dead until he/she is warm and dead. Remarkable accounts of recovery after prolonged cardiac arrest have been reported in patients with hypothermia.[citation needed] It is presumed that this is because the low temperature prevents some of the cellular damage that occurs when blood flow and oxygen are lost for an extended period of time.










